Age-related macular degeneration (ARMD) is a highly prevalent, severely visually disabling disease affecting millions of people worldwide. As its name implies, the disorder affects the macula and therefore central vision, thereby causing significant disability and immeasurable personal impact not only to the patient, but also the family and loved ones caring for those afflicted.
There are two major forms of the disease: atrophic or ‘dry’ macular degeneration and exudative or ‘wet’ ARMD. These are distinguished by the presence in the latter of the proliferation of abnormal new blood vessels, or formation of a choroidal neovascular membrane. The vast majority of patients with ARMD have the atrophic form, commonly presenting with drusen and retinal pigment epithelial (RPE) atrophic changes of the central macula. Although the atrophic form of the disease is much more prevalent, the largest numbers of patients that develop severe visual loss have the exudative form of ARMD.
While the precise cause of the disease remains elusive, many risk factors have been identified that contribute to the complex interaction of genetic and environmental influences that underlie the pathogenesis. More recently, genetic predisposing factors have been investigated and several candidate genes and molecular culprits have been identified.
Many treatment modalities have been employed to halt the progression of macular degeneration. Management for the atrophic form of the disease is aimed at prevention, risk reduction, education, and recognition of more advanced disease. One early treatment modality for exudative ARMD consisted of thermal laser application to choroidal neovascular membranes. While these occasionally resulted in good anatomical results, the visual results were often poor. To the delight of many practitioners and patients, progress has been made over the past decade. Research on drugs capable of stopping abnormal new blood vessel growth led to the development of anti-vascular endothelial growth factors (anti-VEGFs), which are highly successful in halting the progression of both the disease process and visual loss associated with exudative macular degeneration. Furthermore, a large body of research is currently under way to develop new diagnostic and treatment modalities.
Epidemiology
ARMD is the major cause of severe central visual loss in the US in people over 60 years of age.1,2 Overall, the disease appears to be much more common in Caucasians. It is estimated that there are between 15 and 20 million Americans living with at least the earliest signs of ARMD, affecting approximately 18% of Americans between 65 and 74 years of age.3 This figure varies worldwide with lower prevalence in the Asian and African continents. More than eight million people in the US have bilateral intermediate or unilateral advanced disease,4 with approximately 1.75 million Americans having advanced disease.5
Although legal blindness rarely occurs before the seventh or eighth decade of life, over 200 cases per million per year will result in legal blindness, with between 60 and 80% of these cases arising from neovascular ARMD.1–3 The overall prevalence of either neovascular AMD or geographic atrophy in people over 40 in the US is about 1.5%, while the overall prevalence of one or more large drusen is 6.12%.1 As the elderly population in the US is expected to dramatically increase over the next two decades, the number of people affected by ARMD is predicted to rise as well.
Impact on Society
ARMD proves to be a major public health concern, not only because of its current and predicted increased prevalence, but also because of the disabling impact it has on those suffering vision loss as a result of advanced ARMD. ARMD has a dramatic impact on the elderly in terms of daily living and overall quality of life.6,7 Not only are visual impairments associated with difficulty with activities of daily living, but also with increased risk of depression and accidental injury.8,9 In addition, significant occupational impairment may result from even mild visual impairment. Furthermore, elderly patients with blinding disease have higher likelihood of multiple sensory impairments.10,11
Risk Factors
Risk factors for development of ARMD include advancing age, hyperopia, light skin pigmentation, family history, smoking, female gender, hypertension, hypercholesterolemia, and cardiovascular disease.12–19
Pathogenesis and Clinical Manifestations
The pathogenic basis of ARMD is diverse and complex, depending on the stage of disease.20–22 A massive body of research has been undertaken in order to elucidate the genetic and environmental interplay that leads to the development of various stages and phenotypic variations of the disease.
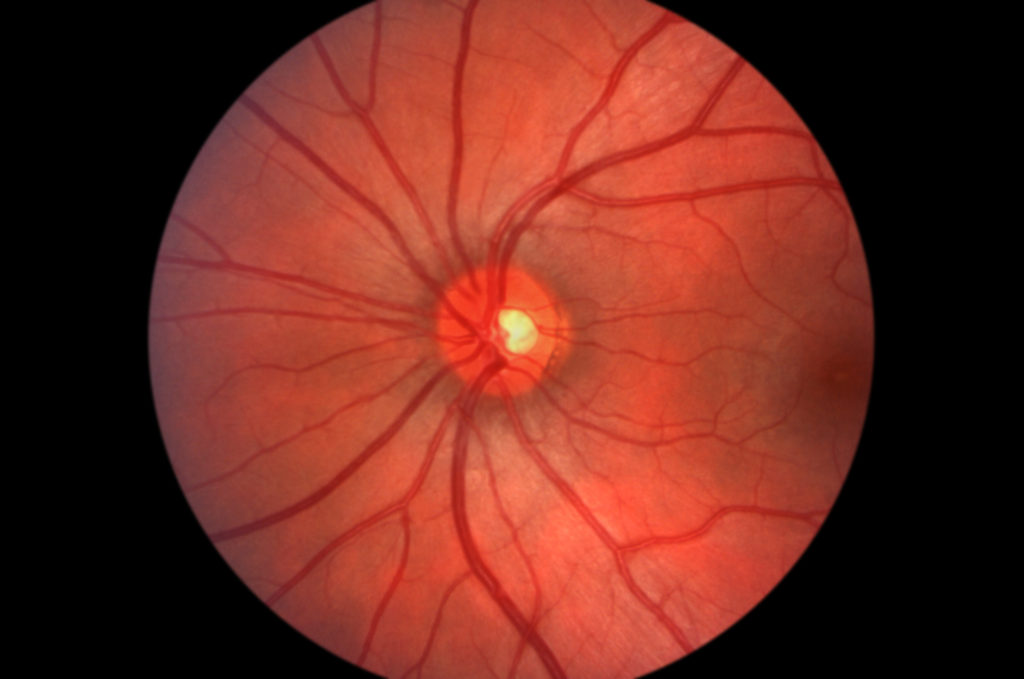
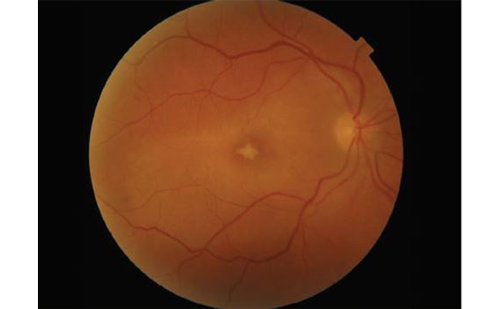
The atrophic form of the disease is characterized by macular RPE alterations, the accumulation of lipofuscin and drusen, retinal pigment epithelial atrophy, and degeneration of segments of the choriocapillaris.23,24 Perhaps the earliest sign of the development of ARMD is the presence of macular drusen, or lipid-rich material with various amounts of collagen fibrils that accumulate at the level of the sub-RPE and Bruch’s membrane25 (see Figure 1).
Pigment changes early in the disease consist of more focal areas of RPE hyperpigmentation and areas of non-contiguous, mottled depigmentation. Histologically, this represents atrophic areas of RPE overlying drusen deposits.26 As atrophic macular degeneration progresses, extensive areas of RPE and retinal atrophy ensue leading to the late stage known as geographic atrophy. This stage is characterized ultrastructurally by RPE loss and damaged photoreceptors in association with abnormal distribution of opsins in degenerating cells,27 with overlying thinning of the neurosensory retina.28 Segments of the choriocapillaris underlying the degenerating RPE become atrophic as well.
Drusen are classified by size, with small drusen considered to be <64µm, intermediate drusen 64–124µm, and large drusen >125µm.24 Larger drusen may give rise to areas of RPE detachment, sometimes referred to as a drusenoid pigment epithelial detachment (PED). Largersized drusen, larger number of drusen, confluence of drusen, and presence of soft drusen have been noted to be associated with more advanced atrophic as well as exudative forms of ARMD.2,29 Clinically, patients with less-severe atrophic macular degeneration most often have few symptoms. However, with the presence of central geographic atrophy, patients can have severe vision loss and central scotoma (blind spot).
Exudative (or wet) macular degeneration is characterized by formation of choroidal neovascular membrane, which occurs when fibrovascular tissue begins to grow from the choroid through Bruch’s membrane, thereby destroying the architecture of the overlying RPE and outer retina. Patients present with variable degrees of metamorphopsia (perception of straight lines appearing wavy), decline in visual acuity, or scotoma. Clinically, examination reveals presence of intra-retinal or subretinal fluid; hemorrhage at any layer (pre-, intra-, or subretinal or sub-RPE); RPE detachment; and/or presence of lipid (see Figure 2). The end-result of untreated neovascularization is fibrotic scar formation, known as a disciform scar, with permanent central vision loss (see Figure 3). Fluorescein angiography, indocyanine green angiography, and optical coherence tomography (OCT) imaging are used to aid in the diagnosis of exudative ARMD.
The specific cascade of events that leads to this wet form of ARMD is complex and continues to be completely elucidated.30 It is thought that focal defects in Bruch’s membrane and oxidative stress may contribute to the pathophysiologic development of choroidal neovascularization. Furthermore, upregulation of pro-angiogenic factors such as VEGF and platelet-derived growth factor (PDGF) or the downregulation of antiangiogenic factors such as pigment epithelial-derived growth factor (PEDF) or endostatin are known to play a major role in the process, and now serve as possible therapeutic targets in the management of exudative ARMD.31,32 Thus, the major event seems to be a disruption in the balance of pro-angiogenic and anti-angiogenic factors. The initiating event in this process remains elusive and is likely diverse. Many soluble factors such as VEGF, hypoxia-inducible factor (HIF), fibroblast growth factor (FGF), PDGF, insulin-like growth factor (IGF) and many others have been shown to have pro-angiogenic properties.30–33 Additionally, there is recent evidence showing that drusen or their components may have some pro-angiogenic effects.34
Genetic Factors
Recently, genetic factors have been investigated, and several candidate susceptibility polymorphisms have been identified. An association with variation in fibulin 5 was demonstrated in patients with ARMD.35 Subsequently, genome-wide linkage analysis led to the identification of several candidate genes.36,37 Polymorphisms on chromosomes 1, 2, 3, 10, and 16 have been identified by several genome-wide scans.38
Complement factor H polymporphism variant on choromosome 1 has a significant association with various stages of ARMD.39–41 Interestingly, this resides within a binding site for cross-reactive protein and is an important regulator of various aspects of the complement cascade. The polymorphism is significantly associated with both neovascular ARMD and geographic atrophy, as well as conferring a higher risk of bilateral disease. More recently, an additional locus on chromosome 10q LOC387715 that confers an independent risk of ARMD has been identified.42 The apparent importance of genes involved in the complement cascade has led to further studies and identification of several additional candidate genes, including complement component 2.43
Although several biologic predispositions are known to exist and continue to be uncovered, the risk and development of ARMD has a highly complex and multifactorial etiology. As we begin to further understand the pathogenesis of the disease more clearly, there appears to be a variety of genetic risk factors that are then modified by environmental risk factors to result in a final common pathway with variable ocular manifestations and phenotypic expression.
Therapy
Dry (Atrophic) Age-related Macular Degeneration
Current therapy of atrophic ARMD revolves around vitamin supplementation to reduce progression. This is compounded with the patient’s overall risk assessment, patient education, avoidance of cigarette smoking, regular follow-up examination schedule, and home monitoring by the patient for new metamorphopsia or scotoma with the aid of an Amsler grid.
The Age-Related Eye Disease Study (AREDS) developed a grading scale for macular degeneration and evaluated the benefit of zinc and antioxidant therapy for preventing vision loss in various stages of AMD.44,45 Patients with intermediate ARMD (defined as a few intermediate or at least one large drusen, or non-central geographic atrophy) or unilateral advanced ARMD (vision loss secondary to ARMD in one eye) were found to benefit from a supplement of antioxidants (500mg vitamin C, 400IU vitamin E, 15mg beta carotene), and zinc (80mg zinc oxide and 2mg cupric oxide to prevent zinc-induced anemia). Results from AREDS showed that those with intermediate or unilateral advanced ARMD who received the above combination of supplements had a 25% risk reduction in the progression to advanced AMD as well as a 19% risk reduction in rates of moderate vision loss (loss of three or more lines of visual acuity) at five years. AREDS 2 is currently under way examining the possible added benefit of lutein, zeaxanthin and omega 3 fatty acids on ARMD progression.
Wet (Exudative) Age-related Macular Degeneration
Neovascular ARMD has been a historically challenging disease to treat. Early treatment modalities included laser photocoagulation to welldefined areas of extrafoveal or juxtafoveal choroidal neovascularization. Subfoveal lesions were poor candidates for laser photocoagulation, given resulting central scotoma as a result of the treatment. In the Macular Photocoagulation Study (MPS), the goal of laser photocoagulation was to decrease the risk of additional visual loss. While this treatment was shown to decrease the risk of severe visual loss (defined as loss of six or more lines of vision or a quadrupling or worse of the visual angle) at five years after treatment,46 patients develop a permanent scotoma. Therefore, except for serving as an option for extrafoveal lesions (that would not leave a central scotoma), this treatment modality has become obsolete in the era of newer therapies.
Photodynamic therapy (PDT), involving the systemic administration of a photosensitive agent (e.g. verteporfin) followed by activation via sensitizing light, was investigated in order to treat subfoveal neovascularization. The Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) and Verteporfin in Photodynamic Therapy (VIP) trials provided the basis for the use of verteporfin PDT in treating ARMD, as PDT was shown to reduce the risk of severe visual loss for certain types of choroidal neovascular membrane.47,48 Since the advent of anti-VEGF agents, PDT has fallen out of favor as primary treatment, but is used in combination with anti-VEGF agents and/or steroids for lesions recalcitrant to anti-VEGF agents alone.
Currently, the first-line management for choroidal neovascularization in ARMD is anti-angiogenic therapy. Three anti-VEGF agents have been used in the treatment of exudative ARMD, two of which are US Food and Drug Administration (FDA) approved for use in macular degeneration (pegaptanib sodium and ranibizumab), with the third being used off-label in the treatment of ARMD (bevacizumab). The currently available mode of delivery of all these agents is repeated intra-vitreal injection.
Pegaptanib sodium (Macugen; OSI/Eyetech, Inc., Melville, NY) is an RNA aptamer that binds specifically only to VEGF isoform 165. Injection of pegaptanib every six weeks was shown to result in a significant reduction in severe visual loss for subfoveal neovascularization in the VEGF Inhibition Study In Ocular Neovascularization (VISION), with 70% of treated patients losing fewer than three lines of vision compared with 55% of those receiving sham injection.49 Pegaptanib was approved by the FDA for ARMD treatment in 2004, but is not used with the availability of other anti-VEGF agents with a more potent effect.
Ranibizumab (Lucentis; Genentech, Inc., San Francisco, CA) is a nonselective recombinant humanized monoclonal antibody fragment that inhibits all VEGF-A isoforms, and is derived from the same parent murine antibody as bevacizumab (Avastin; Genentech, Inc.). The Minimally Classic/Occult Trial of the Anti-VEGF Antibody Ranibizumab in the Treatment of Neovascular AMD (MARINA) and Anti-VEGF Antibody for the Treatment of Predominantly Classic CNV in AMD (ANCHOR) trials provided data for FDA approval of ranibizumab in the treatment of all subtypes of exudative ARMD.50,51 Most importantly, these trials were the first to show an improvement in vision in patients treated for ARMD.
In the MARINA trial, 95% of subjects at 12 months and 90% at 24 months receiving monthly ranibizumab injections lost fewer than three lines of vision compared with 62 and 53%, respectively, receiving sham injections. Furthermore, 34% at 12 months and 33% at 24 months gained three or more lines of vision compared with 4 and 5% receiving sham injections.50 In the ANCHOR trial, 96% of subjects at 12 months and 90% at 24 months receiving monthly ranibizumab injections lost fewer than three lines of vision compared with 64 and 66%, respectively, receiving PDT. Furthermore, 40% at 12 months and 41% at 24 months gained three or more lines of vision compared with 6% at both 12 and 24 months receiving PDT.51,52
Bevacizumab is FDA-approved for use in metastatic colorectal, lung, and breast cancer, and is being used off-label for the treatment of ARMD. Since the first report of its use in the treatment of ARMD, numerous retrospective and prospective studies have shown its effectiveness in treating exudative ARMD.53–55 The agent appears to be safe and effective for intra-vitreal use56,57 and has gained popularity given its significantly lower cost compared with ranibizumab.
A variety of dosing intervals for bevacizumab and ranibizumab have been studied, but there remains no consensus as to the most desirable treatment strategy for the use of anti-VEGF agents in the treatment of exudative ARMD, although treatment based on OCT imaging seems beneficial.55,58,59 Combination therapies involving intravitreal corticosteroids,60,61 PDT and anti-VEGF agents are being increasingly researched for potential synergistic effects or for use in recalcitrant disease.
Future therapies being investigated include blocking the effects of VEGF by different mechanisms, such as a decoy receptor with VEGF trap (Regeneron Pharmaceuticals, Tarrytown, NJ); small interfering RNA (siRNA) agents that downregulate the VEGF or VEGF receptor genes (e.g. bevasiranib (OPKO Health, Inc./Acuity Pharmaceuticals, Miami, FL) and AGN211745 (Allergan, Inc., Irvine, CA); and focal strontium-90 beta radiation delivered via the Epi-Rad 90 Ophthalmic System (NeoVista, Fremont, CA).
In summary, ARMD remains a significant public health concern and important cause of blindness in the elderly. Recent research has focused on the genetic factors responsible for the pathogenesis of ARMD. ARMD presents in either the atrophic form, which is mainly managed with close monitoring and antioxidant and zinc therapy, or the exudative form, for which there is currently effective treatment with anti-VEGF agents. Future therapies are being researched to target both the atrophic and exudative forms of ARMD.